Is a Pharmacist a Doctor? Understanding the PharmD Degree and Clinical Roles
What if the most overqualified member of your healthcare team is the one you see most often, yet understand the least? You’ve likely noticed the ‘Doctor’ title on a white coat at your local pharmacy and felt a flicker of uncertainty about what it actually means for your care. It’s frustrating to sort through conflicting reports about ‘scope creep’ while simply trying to figure out who has the final word on your prescription’s safety. To settle the common question, is a pharmacist a doctor, we’re diving into the reality of the Doctor of Pharmacy (PharmD) degree, which became the mandatory entry level standard in the United States in 2004. You’ll discover the grueling academic requirements that involve four years of professional study after a rigorous pre-medical track.
This guide clarifies the distinct boundaries between the PharmD and the MD, highlights the 1,740 hours of required clinical experience, and identifies the specific scenarios where a pharmacist’s expertise is your most valuable asset. By the end, you’ll have a clear map of the pharmacy professional’s role in modern medicine and the confidence to utilize their clinical knowledge for your health goals.
Key Takeaways
- Understand why the answer to “is a pharmacist a doctor” is a definitive yes in the modern healthcare landscape and how the PharmD degree establishes this professional authority.
- Explore the evolution of pharmacy education and why the transition from a bachelor’s degree to a doctorate was necessary to manage increasingly complex drug therapies.
- Learn the critical distinctions between medical doctors and pharmacists, specifically comparing the focus on diagnosis versus the mastery of pharmacotherapy.
- Discover the expanding clinical roles of pharmacists in high-stakes environments like the ICU and the importance of Board Certification in specialized practice.
- Identify the rigorous path to licensure, including the specific examinations required to ensure professional competence and legal compliance in the field.
Defining the Title: Is a Pharmacist a Doctor?
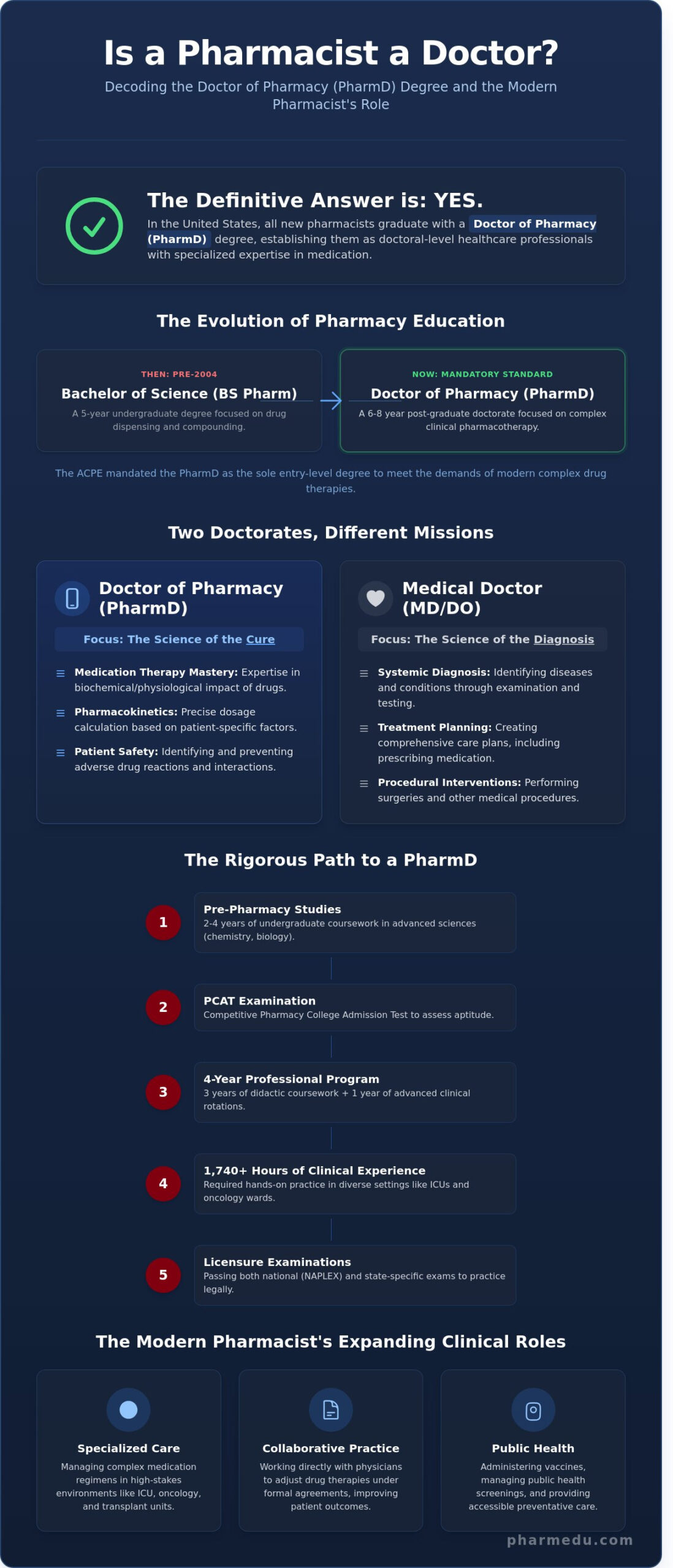
Yes, in the United States, all entry-level practitioners now earn a clinical doctorate. When patients ask is a pharmacist a doctor, the answer depends on whether they’re referring to an academic degree or a specific medical role. Since 2000, the American Council on Pharmaceutical Education (ACPE) has mandated the Doctor of Pharmacy (Pharm.D.) as the minimum educational standard for licensure. This shift moved the profession away from the traditional five-year Bachelor of Science (BS Pharm) to a rigorous four-year post-graduate program.
Distinguishing between a Medical Doctor (MD) and a Doctor of Pharmacy is essential for clinical clarity. MDs and Doctors of Osteopathic Medicine (DO) prioritize systemic diagnosis and surgical or procedural interventions. Conversely, a PharmD focuses on the biochemical and physiological impact of medications. In a hospital setting, the title “Doctor” reflects this clinical expertise in pharmacotherapy. In retail environments, practitioners often use the title “Pharmacist” to prevent patients from seeking a primary diagnosis where a medication review is actually occurring. Understanding is a pharmacist a doctor requires recognizing that their expertise lies in the science of the cure rather than the initial diagnosis of the disease.
Academic vs. Clinical Titles
The term “Doctorate” signifies a high level of academic achievement. Separate the profession from the credential. “Pharmacist” is the job title, while “PharmD” is the degree earned. This mirrors the evolution of other healthcare fields. For example, Physical Therapists now earn a DPT (Doctor of Physical Therapy) and many nurses pursue a DNP (Doctor of Nursing Practice). These degrees require roughly 1,740 hours of clinical rotations to ensure practitioners can handle complex patient cases effectively.
The Legal Standing of the PharmD
State licensing boards recognize the PharmD as the authoritative credential for managing medication therapy. This doctoral-level education provides the legal basis for expanded roles, such as administering vaccines or entering collaborative practice agreements. While the US fully adopted this model by 2000, international standards vary. The United Kingdom and much of Europe still primarily utilize the Master of Pharmacy (MPharm) or Bachelor’s degrees; however, they’re increasingly exploring doctoral pathways to match modern healthcare demands.
The Evolution of Pharmacy Education: From RPh to PharmD
To understand whether a pharmacist is a doctor, you’ve got to look at the educational overhaul that reshaped the profession. For decades, a five-year Bachelor of Science in Pharmacy (BSPharm) was the standard. However, as drug therapies became more targeted and complex, the healthcare system required a higher level of clinical expertise from those managing these substances. This led to a complete restructuring of how pharmacists are trained and perceived in the medical community.
Why the Bachelor’s Degree Disappeared
The turning point arrived in 2000. The Accreditation Council for Pharmacy Education (ACPE) issued a mandate that made the PharmD the only accredited degree for new pharmacy students in the United States. This didn’t invalidate the titles of existing practitioners. Thousands of Registered Pharmacists (RPh) who held bachelor’s degrees were grandfathered in, allowing them to continue practicing without returning to school. The PharmD was created to address the ‘medication explosion’ of the late 20th century. As the number of FDA-approved molecular entities grew significantly, the role of the pharmacist had to transition from manual compounding to complex clinical decision-making.
The Rigor of a PharmD Program
Earning a PharmD isn’t a shortcut. It requires six to eight years of rigorous university study. Most candidates start with the Pharmacy College Admission Test (PCAT), a competitive entry exam that filters for high aptitude in chemistry and biology. Once admitted, students face three years of intense didactic coursework followed by a final year of Advanced Pharmacy Practice Experiences (APPEs). These rotations involve 1,600 to 2,000 hours of direct clinical work in diverse settings like intensive care units and oncology wards.
The core curriculum focuses heavily on pharmacokinetics and Evidence-Based Medicine (EBM). Students learn to calculate precise dosages based on a patient’s renal function or genetic profile. This level of training is why, when someone asks is a pharmacist a doctor, the answer is a definitive yes in terms of academic achievement. Maintaining this high standard requires constant effort; many practitioners rely on structured professional development to keep their clinical skills sharp and meet credit requirements. The shift to a doctoral standard ensures every pharmacist is equipped to be a primary safeguard in modern healthcare. For a detailed breakdown of every academic and regulatory milestone involved, the pharmacist education requirements guide for 2026 offers a comprehensive step-by-step roadmap aligned with current board standards.
Pharmacist vs. Physician: Clearing Up the Misconceptions
While both professionals hold doctoral degrees, their daily responsibilities follow distinct clinical paths. Physicians primarily focus on the diagnostic process, identifying illnesses through physical exams and lab results. Pharmacists specialize in pharmacotherapy, ensuring that the chosen treatment is safe, effective, and tailored to the patient’s unique physiology. This distinction often leads people to ask, “is a pharmacist a doctor?” in the same sense as a GP. The answer lies in their specialized expertise rather than a hierarchy of care.
Educational paths reflect these different goals. A medical student typically completes 4,000 to 6,000 clinical hours before graduation. PharmD students complete approximately 1,500 to 2,000 hours of Advanced Pharmacy Practice Experiences (APPEs). These roles aren’t meant to compete; they’re designed to be synergistic. A 2022 study published in the Journal of the American Board of Family Medicine showed that physician-pharmacist collaboration reduced medication errors by 34%.
Training and Residency Differences
Medical residents spend 3 to 7 years in intensive post-graduate training to master surgery or internal medicine. Pharmacy residencies are optional and usually last 1 to 2 years, focusing on niche areas like oncology or infectious diseases. Pharmacists earn the title of the “most accessible healthcare provider” because 90% of Americans live within five miles of a community pharmacy. They provide immediate professional consultations without the weeks-long wait times often associated with specialist physicians.
Prescribing Authority and Collaborative Practice
The myth that pharmacists can’t prescribe is outdated. Through Collaborative Practice Agreements (CPAs), pharmacists manage drug therapy under a protocol with a physician. In states like California and Oregon, pharmacists have independent prescribing authority for hormonal contraceptives and smoking cessation aids. Their intervention is critical in managing polypharmacy. Since 40% of seniors take five or more prescriptions daily, pharmacists act as the final safety check against dangerous drug-drug interactions that a busy diagnostic clinic might overlook.
- Physicians: Focus on diagnosis and pathology.
- Pharmacists: Focus on chemistry, dosage, and drug interactions.
- Synergy: Pharmacists provide the “how” to the physician’s “what”.
The Clinical Authority of Modern Pharmacists
Modern healthcare relies on pharmacists far beyond the traditional retail setting. They don’t just fill prescriptions; they direct therapy. When patients ask, is a pharmacist a doctor, the answer in a clinical setting is often found at the bedside in the ICU or the oncology ward. These professionals serve as primary consultants for physicians, ensuring that complex drug regimens are both safe and effective. They’ve moved from the back of the store to the front lines of patient care.
Specialized Pharmacy Roles
Clinical pharmacists are now integral members of multidisciplinary teams. In the ICU, critical care pharmacists manage life-saving drips and titrate medications in real-time. Infectious disease pharmacists lead antibiotic stewardship programs. These programs are vital; a 2021 study indicated they can reduce hospital-acquired infections by 31%. In ambulatory care, pharmacists manage chronic conditions like hypertension and diabetes, often possessing the authority to adjust dosages independently under collaborative practice agreements. This autonomy proves that the question is a pharmacist a doctor is rooted in their evolving clinical responsibility.
Board Certification: The ‘Specialist’ Pharmacist
The Board of Pharmacy Specialties (BPS) offers the gold standard for clinical recognition. Obtaining a BCPS (Board Certified Pharmacotherapy Specialist) credential requires rigorous training and a high-stakes examination. This certification bridges the gap between a general PharmD and a specialized clinical doctor. To maintain these credentials, pharmacists must complete 100 hours of continuing education every seven years or pass a recertification exam. This commitment to lifelong learning ensures they remain at the forefront of pharmacological science.
The impact of these specialists is measurable. A 2022 report published in the Journal of the American College of Clinical Pharmacy found that pharmacist-led interventions reduced 30-day hospital readmission rates by 22%. They act as internal medicine consultants, catching drug-drug interactions that might otherwise lead to patient harm. Their expertise transforms the healthcare landscape into a collaborative environment where medication safety is the priority.
Mastering the Path: How to Become a Doctor of Pharmacy
Completing a PharmD program is a massive achievement, but the journey to clinical practice involves clearing final regulatory hurdles. While the degree confirms academic status, state licensure requires passing the North American Pharmacist Licensure Examination (NAPLEX) and the Multistate Pharmacy Jurisprudence Examination (MPJE). These exams ensure that every practitioner possesses the clinical acumen and legal knowledge to protect public health. The question is a pharmacist a doctor finds its true answer here; the title is validated through these rigorous assessments of competency and safety.
- NAPLEX: A 225-question exam focusing on patient safety, drug characteristics, and clinical outcomes.
- MPJE: A state-specific exam testing the legal requirements of pharmacy practice and controlled substance regulations.
- Clinical Rotations: Final-year students complete roughly 1,440 to 1,600 hours of supervised practice before graduation.
Preparing for the NAPLEX
The NAPLEX remains a formidable barrier, with pharmacology sections historically being the most difficult for candidates. This section requires a deep understanding of drug mechanisms, contraindications, and complex dosing calculations. PharmEDU simplifies this process for students. Our platform utilizes high-yield video vignettes and interactive tools designed to boost retention rates by 60% compared to standard textbook reading. If you’re ready to secure your clinical credentials, the NAPLEX prep course provides the structured, evidence-based support needed to master these high-stakes topics.
The Future of the Profession
Pharmacy is moving far beyond the traditional dispensing counter. By early 2024, approximately 40 U.S. states have made significant legislative strides toward “Provider Status” for pharmacists. This shift allows doctors of pharmacy to manage chronic conditions, order lab tests, and receive reimbursement for clinical consultations. It’s a pivotal moment to enter the field. While your current pharmacology coursework might feel overwhelming, these details are the tools you’ll use to improve patient outcomes. This evolution reinforces why is a pharmacist a doctor is a question of growing importance in the modern healthcare team.
The “Doctor” designation reflects a commitment to lifelong learning and precision. Success in this field requires more than just passing an initial test; it demands staying updated on 50+ new drug approvals annually and shifting federal regulations. PharmEDU acts as your digital mentor, turning mandatory continuing education into a genuine professional advantage. Your title isn’t just a prefix on a lab coat. It’s a promise of safety and expertise that you fulfill every time you intervene to prevent a medication error or optimize a patient’s therapy plan. For those considering this career path, our comprehensive guide on how to become a pharmacist provides detailed insights into the educational requirements, licensing process, and career opportunities available in this evolving field.
Advancing Your Clinical Expertise in Modern Pharmacy
The transition of pharmacy education has fundamentally reshaped the healthcare landscape. Since 2000, the Doctor of Pharmacy (PharmD) has served as the mandatory entry-level degree, ensuring practitioners complete a rigorous four-year professional program. When a patient asks is a pharmacist a doctor, the answer reflects their deep expertise in biochemical mechanisms and clinical outcomes. While they don’t diagnose like physicians, their role as the final check in medication safety is indispensable for modern patient care.
Achieving this level of clinical mastery demands reliable, high-quality resources. PharmEdu supports your professional growth with a platform built by healthcare educators specifically for healthcare students. You can access over 100 high-yield pharmacology topics and sharpen your skills with board-style practice quizzes and interactive flashcards. We’ve designed these tools to simplify complex regulations and scientific data, letting you focus on providing excellent care.
Start Your Journey to Mastering Pharmacology with PharmEDU
Your dedication to professional excellence ensures a safer, more effective healthcare system for everyone.
Frequently Asked Questions
Can a pharmacist legally be called ‘Doctor’ in a hospital?
Yes, a pharmacist holding a Doctor of Pharmacy degree is legally entitled to use the title “Doctor” in clinical settings. While they use the “Dr.” prefix, hospital protocols often require them to identify as a pharmacist to prevent patient confusion with medical doctors. This professional recognition reflects the 4,000 to 6,000 hours of clinical training required to earn the degree.
Is a PharmD the same as a PhD in Pharmacology?
No, a PharmD is a professional clinical degree focused on patient care, while a PhD in Pharmacology is a research doctorate centered on drug discovery. PharmD students complete 1,740 hours of practical rotations to prepare for healthcare roles. PhD candidates spend 4 to 6 years conducting laboratory research and defending a dissertation to advance scientific knowledge.
How many years does it take to become a pharmacist doctor?
It typically takes 6 to 8 years of rigorous university education to answer the question: is a pharmacist a doctor? Students spend 2 to 4 years on undergraduate prerequisites followed by a 4-year professional PharmD program. After graduation, 30% of pharmacists pursue an additional 1 or 2 years of residency to specialize in areas like oncology.
What is the difference between a pharmacist and a pharmacologist?
Pharmacists focus on direct patient care and medication management in community or hospital settings. Pharmacologists work in laboratories or for pharmaceutical companies, studying how chemical compounds interact with biological systems. While a pharmacist needs a license to practice, a pharmacologist focuses on the 10 to 15-year development cycle of new medications in a research capacity.
Can pharmacists prescribe medication like a doctor?
Pharmacists can prescribe medications in 49 states through Collaborative Practice Agreements with physicians. In states like California and New Mexico, “Advanced Practice Pharmacists” have expanded authority to initiate or adjust drug therapy for patients. They don’t have the same broad diagnostic powers as an MD, but they manage complex regimens for chronic conditions like diabetes.
Do all pharmacists have to get a PharmD now?
All new pharmacy graduates in the United States have been required to earn a PharmD degree since the year 2000. Pharmacists who earned a 5-year Bachelor of Pharmacy before this transition are still licensed to practice and aren’t required to return to school. Current data shows that over 90% of the active workforce now holds a doctorate to meet modern accreditation standards.
Why did the pharmacy degree change from a Bachelor’s to a Doctorate?
The American Council on Pharmaceutical Education mandated the shift to a doctorate in 1992 to prepare pharmacists for clinical decision-making. Modern healthcare requires expertise in pharmacogenomics and complex drug interactions that a 5-year bachelor’s degree couldn’t fully cover. This change ensures that when patients ask is a pharmacist a doctor, the answer reflects their role as high-level clinical consultants.
What is the NAPLEX exam and why is it required for pharmacists?
The NAPLEX is a 225-question standardized exam that measures a candidate’s knowledge of pharmacotherapy and safe medication preparation. It’s a mandatory requirement for licensure in all 50 U.S. states to ensure a minimum competency level for public safety. Candidates must pass this 6-hour computer-based test to prove they can safely manage the 4.5 billion prescriptions filled annually in the U.S.







